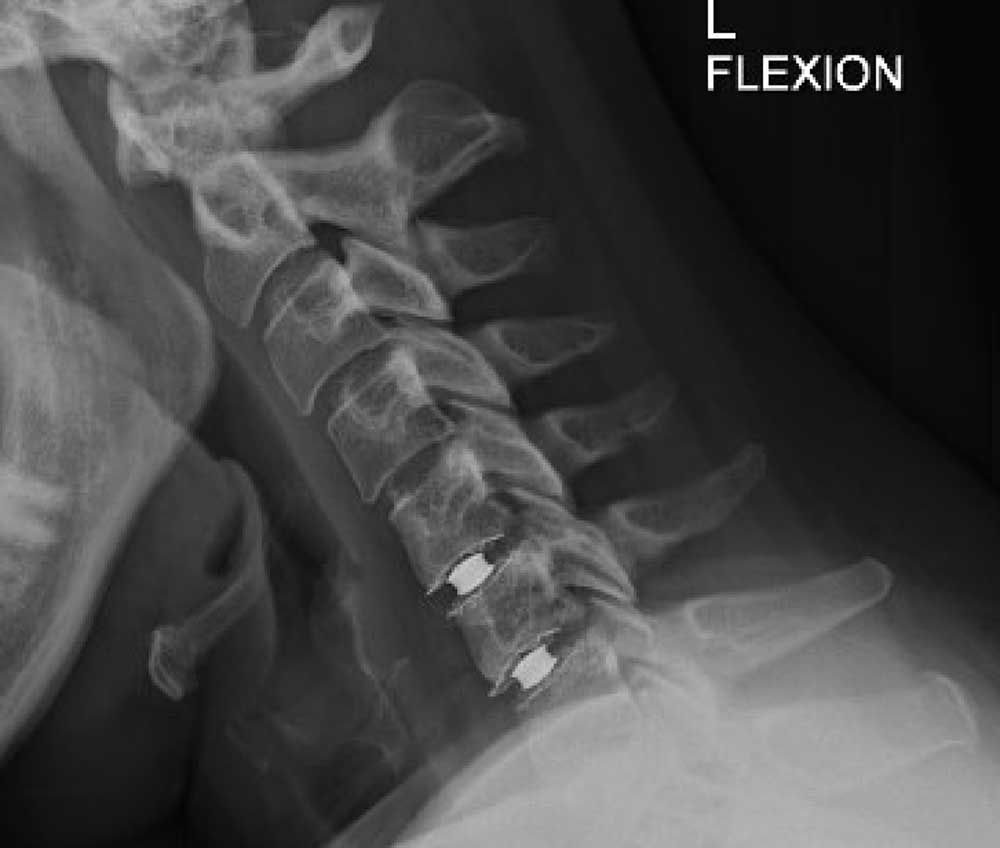
Cervical Arthroplasty Considerations
Cervical arthroplasty (disc replacement) is a surgical procedure that replaces a damaged or degenerated disc in the neck with an artificial device. Unlike spinal fusion, which immobilizes the affected segment of the spine, cervical arthroplasty aims to preserve some degree of motion and flexibility. This motion and flexibility may have some advantages for the patient’s quality of life and long-term outcomes…, particularly in the case of younger or more physically active patients. Cervical arthroplasty is not suitable for everyone. In this article, we will explore the indications and contraindications for this innovative treatment, as well as the risks and benefits involved. We will also examine the scientific evidence behind cervical arthroplasty and compare it with other alternatives. Our goal is to provide you with a clear and comprehensive understanding of this procedure, so you can make an informed decision about your health.
Cervical arthroplasty is one of the most recent spinal treatment innovations that has been approved by the FDA. Dr. Goldstein has been directly involved in a number of the investigations of cervical arthroplasty. Since the first approval in 2007, several types of artificial discs have been developed, tested, and ultimately approved. The basic design of a cervical artificial disc consists of two endplates that attach to the adjacent vertebrae and a movable/flexible core between them that allows motion. The core can be made of different materials, such as polyethylene, ceramic, or metal. The endplates can also vary in shape, size, and coating. The aim of these variations is to optimize the biomechanical performance, durability, and compatibility of the artificial disc.
Cervical arthroplasty is indicated for patients who have symptomatic cervical radiculopathy or myelopathy caused by disc pathology at one or two levels between C3 and C7, and who have failed conservative management. The disc pathology can include herniated nucleus pulposus, spondylosis, stenosis, or segmental instability. Cervical arthroplasty aims to relieve the compression of the spinal cord or nerve roots by removing the diseased disc and restoring the disc height and lordosis. By preserving motion at the operated level, cervical arthroplasty may also prevent or delay the development of adjacent segment degeneration, which is a common complication of spinal fusion.
Cervical arthroplasty is contraindicated for patients who have any of the following conditions that may compromise the success or safety of the procedure.
- Advanced degenerative disease of the facet joints with associated neck pain
- Ossification of the posterior longitudinal ligament and/or significant spondylosis
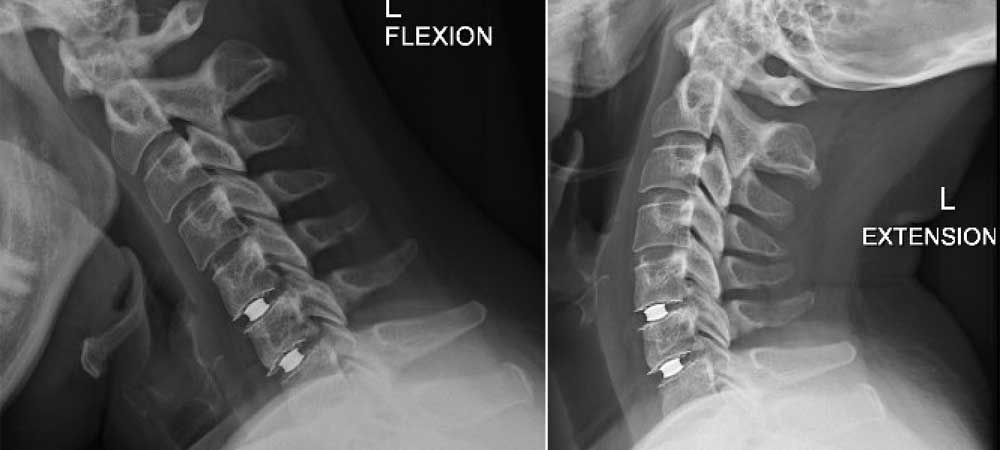
- Pre-operative instability on dynamic flexion-extension images
- Systemic bone illness (osteoporosis, osteopenia, or metabolic bone disease)
- Known allergy to the implant’s materials (PEEK, ceramic, or titanium)
- Infection or inflammation in the cervical spine or adjacent tissues
- Morbid obesity or poor general health
Success Rates for Cervical Arthroplasty
Cervical arthroplasty has been shown to be a safe and effective treatment for cervical disc degeneration with radiculopathy and/or myelopathy. Numerous studies have compared cervical arthroplasty with spinal fusion and found that both procedures provide similar or better outcomes in terms of pain relief, function, and quality of life. However, cervical arthroplasty has some advantages over spinal fusion, such as preserving motion, reducing stress on adjacent levels, and lowering the risk of reoperation.
According to a 2019 review of the literature, the overall success rate of cervical arthroplasty at 10 years was 81%, compared with 66% for spinal fusion. The rate of secondary surgery at adjacent levels was also significantly lower for cervical arthroplasty, 4.7%, versus 16.8% for spinal fusion. These results suggest that cervical arthroplasty is a durable and superior option for patients with cervical disc degeneration.
How to Make an Appointment
If you are suffering from neck pain, arm pain, or other symptoms of cervical disc degeneration, you may be a candidate for cervical arthroplasty. This innovative procedure can help you restore your neck function and improve your quality of life. However, not everyone is eligible for this surgery, and there are some risks and complications involved. Therefore, it is important to consult with a qualified and experienced spine surgeon who can evaluate your condition and recommend the best treatment for you.
Dr. Goldstein has been a leader in the introduction of cervical arthroplasty to the United States and was one of the original investigators of Cervical Artificial Discs in America and played an instrumental role in their becoming mainstream. To explore whether you might be a candidate for this procedure, please contact our office.
For more information on types of Cervical Discs, you can visit implant device websites to learn more about specific technologies.

Cervical Disc Arthroplasty - Spine - Orthobullets
Cervical and Lumbar Spinal Arthroplasty: Clinical Review | American Journal of Neuroradiology (ajnr.org)
Cervical Artificial Disc Replacement Outcomes at 5 to 10 Years (medcentral.com)